For physiotherapists managing patients with severe chronic obstructive pulmonary disease (COPD), the focus often centers on pharmacological adherence, secretion clearance, and general aerobic conditioning. However, the mechanical constraints imposed by the disease—specifically the coexistence of chest wall hypomobility and lung hyperinflation—create a vicious cycle that severely compromises respiratory muscle function. A recent Randomized Controlled Trial (RCT) published in Respirology (2025) offers compelling evidence that manual therapy targeting the chest wall and thoracic spine can significantly enhance respiratory efficiency and functional capacity in this population.
Addressing the Mechanical Constraint
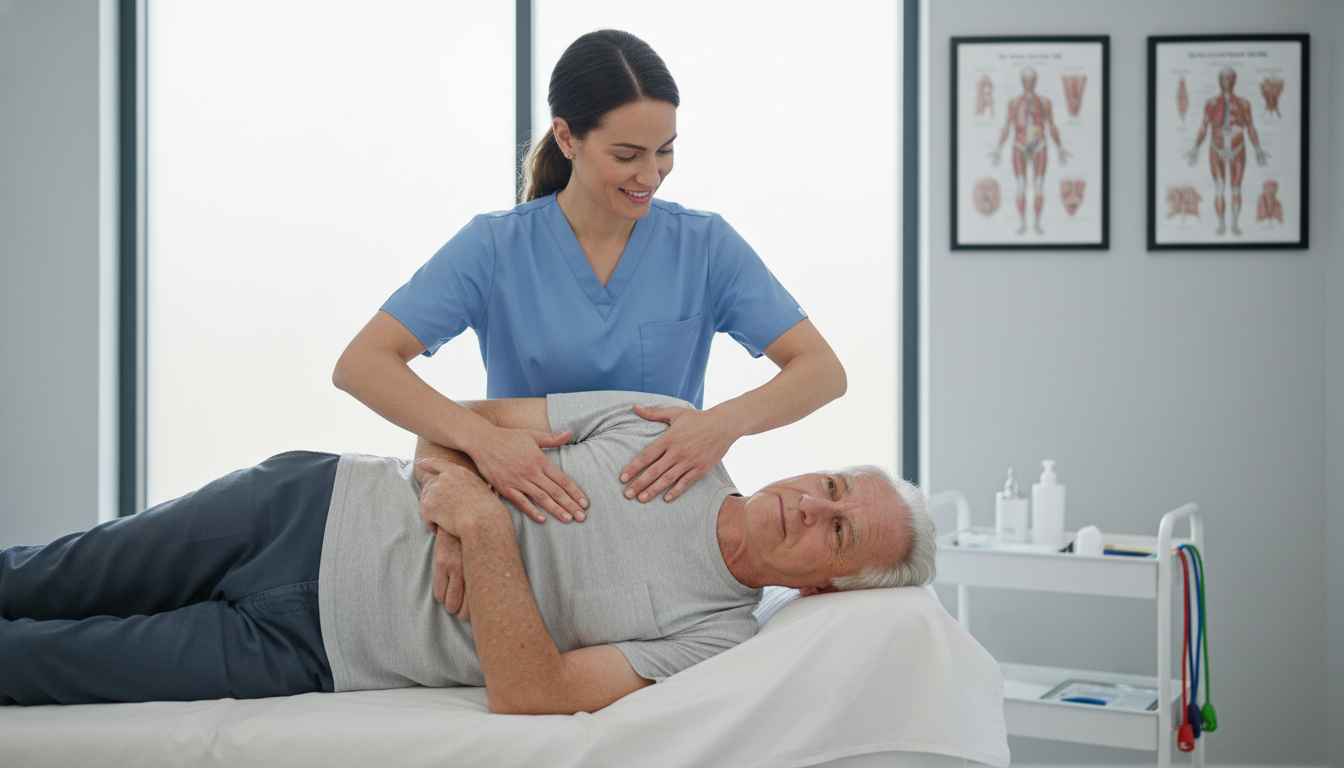
In severe COPD, air trapping leads to a barrel-chest deformity, placing the diaphragm in a flattened, disadvantaged position. Consequently, patients rely heavily on accessory muscles (scalenes, sternocleidomastoid) even at rest. The study by Tsui et al. investigated whether restoring mobility to the rigid thoracic cage could alleviate this burden. The researchers recruited thirty male adults with severe COPD and randomized them into a Chest Wall Mobilization Group (CWMG) and a Control Group (CG). While both groups received standardized education and walking exercises, the CWMG underwent a 6-week protocol (twice weekly) including specific mobilization of the chest wall and thoracic spine.
Significant Gains in Functional Capacity
The results of this RCT are clinically significant for orthopedic and respiratory therapists alike. Following the 6-week intervention, the mobilization group demonstrated a remarkable increase in exercise tolerance. Metabolic equivalents (METs) jumped from less than 3 to a range of 4–6 (p = 0.000). To put this in perspective, this shift represents a transition from very light activity limitations to being able to perform moderate functional tasks, a crucial improvement for quality of life.
Physiological Changes: EMG and Oxygen Extraction
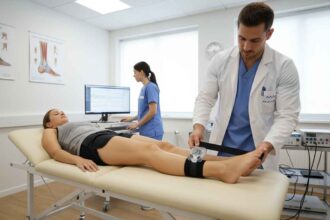
Beyond functional outcomes, the study utilized electromyography (EMG) and near-infrared spectroscopy (NIRS) to understand the physiological mechanisms at play. The data revealed a significant decrease in the activity of the scalene, sternocleidomastoid, and intercostal muscles during incremental cycle testing in the mobilization group compared to controls (p < 0.01). This suggests a restoration of more efficient respiratory mechanics, reducing the neural drive required by accessory muscles to maintain ventilation.
Furthermore, the study noted a significant decrease in tissue oxygen saturation (StO2) and a steeper decline in the oxygenation dissociation slope in the intercostal muscles of the CWMG. This indicates an improved ability of the respiratory muscles to extract and utilize oxygen during physical exertion.
Clinical Implications
The maintenance of these positive results at the 3-month follow-up underscores the potential long-term benefits of integrating manual therapy into pulmonary rehabilitation. For clinicians, this evidence suggests that treating the “pump” (the thoracic cage) via mobilization is a valid and effective adjunct to treating the “lung” (aerobic exercise and medication). By reducing chest wall stiffness, we may lower the work of breathing and unlock functional capacity in patients who were previously limited by mechanical inefficiency.
References
Tsui, A. Y. Y., Cheing, G. L. Y., Chau, R. M. W., Mok, T. Y. W., Ling, S. O., Kwan, C. H. Y., & Tsang, S. M. H. (2025). Benefits of chest wall mobilization on respiratory efficiency and functional exercise capacity in people with severe chronic obstructive pulmonary disease (COPD): A randomized controlled trial. Respirology. Advance online publication.