Chronic Obstructive Pulmonary Disease (COPD) is widely recognized as a multicomponent pathology. While airflow obstruction is the primary hallmark, systemic manifestations—particularly skeletal muscle dysfunction—play a pivotal role in limiting functional capacity. For physiotherapists working in pulmonary rehabilitation, Inspiratory Muscle Training (IMT) is a cornerstone intervention. However, new research published in Physiotherapy Research International (2026) suggests that the intensity of this training requires careful titration to avoid inadvertent hemodynamic consequences.
The Systemic Impact of Respiratory Effort
The physiological connection between the respiratory pump and locomotor muscles is governed, in part, by the inspiratory muscle metaboreflex. When the diaphragm fatigues or works under high loads, a sympathetic reflex constricts peripheral vasculature to shunt blood flow toward the vital respiratory muscles. This phenomenon, known as the "blood steal" effect, can compromise perfusion to the limb muscles, exacerbating exercise intolerance.
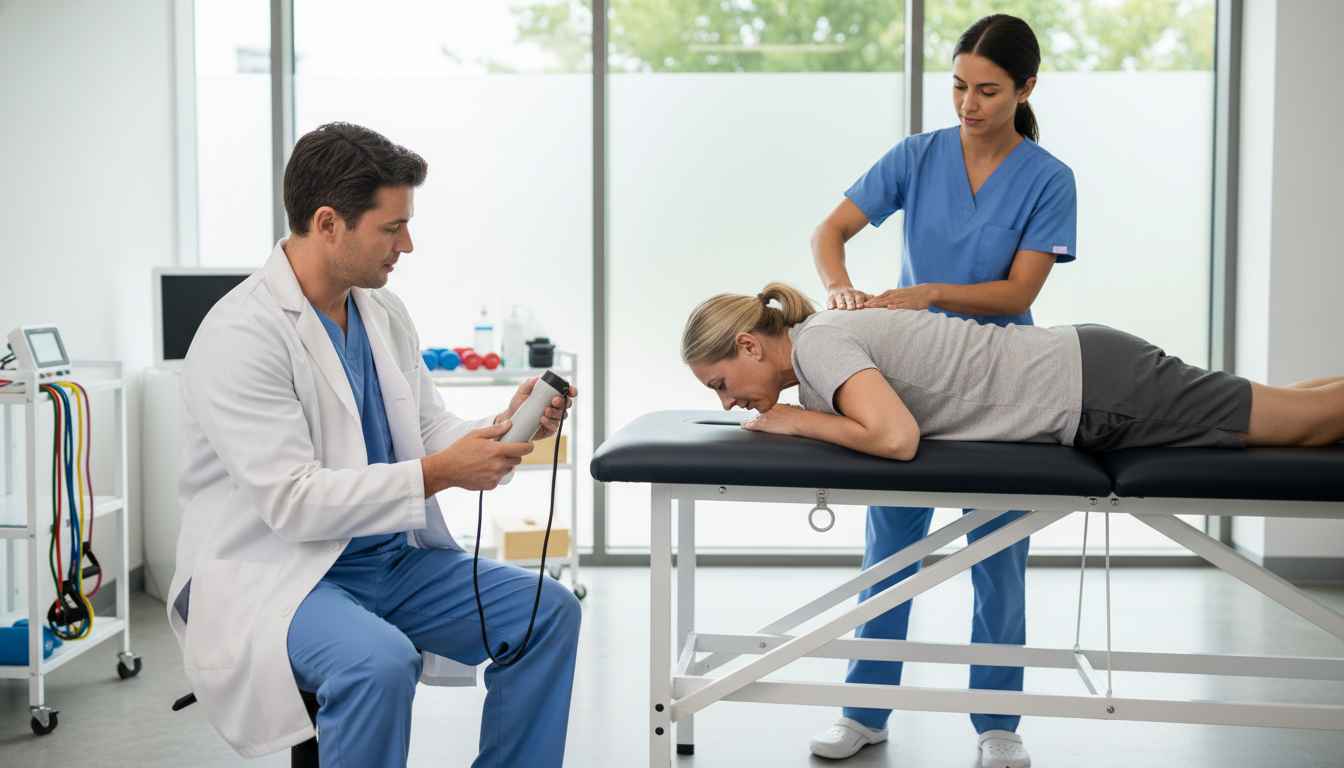
A recent randomized crossover study by Borges et al. investigated this mechanism by analyzing the acute effects of different IMT intensities on peripheral tissue oxygenation. Using near-infrared spectroscopy (NIRS), the researchers monitored the gastrocnemius muscle oxygenation in 29 individuals with COPD during three distinct protocols: high-load IMT (Strength, 60% of maximal inspiratory pressure [MIP]), low-load IMT (Endurance, 30% MIP), and a sham protocol.
Analyzing the Hemodynamic Response
The study yielded critical insights into how training load influences peripheral perfusion. The results indicated that the high-load protocol (IMT-Strength) resulted in a significantly shorter oxygen desaturation time compared to other groups. Essentially, when patients trained at 60% of their MIP, the metabolic demand of the respiratory muscles likely triggered the metaboreflex, accelerating the reduction of oxygen availability in the calf muscles.
This response was particularly pronounced in patients with advanced disease severity (GOLD stages 3 and 4). Although not statistically significant across the entire cohort, the trend suggested that those with severe obstruction experienced a higher rate of peripheral oxygen desaturation during strength-based IMT. Conversely, the low-load protocol (IMT-Endurance) appeared to maintain or even improve peripheral perfusion dynamics, evidenced by favorable differences in mean final tissue oxygen saturation.
Clinical Implications for Prescription
For the clinician, these findings underscore the importance of precision dosing in pulmonary rehabilitation. While high-intensity IMT is effective for increasing diaphragmatic strength, it may acutely compromise peripheral muscle oxygenation in patients with limited physiological reserve. This could theoretically induce earlier limb fatigue or limit the patient’s ability to perform concurrent peripheral muscle training.
The authors conclude that endurance-based IMT (approx. 30% MIP) may be a hemodynamically safer entry point for patients with severe COPD or those exhibiting signs of early metabolic fatigue. Clinicians should consider monitoring signs of peripheral perfusion and fatigue when implementing high-intensity protocols, ensuring that the benefits of respiratory strengthening do not come at the cost of peripheral ischemia.
References
Borges, N. M. D. S., Lima, D. T., Morais, A. B. A., Tenório, L. N. F. C., Vieira, S. T., Carneiro, H. M. L. O., Freitas, A. L., Silva, D. F. S., Silva, E. D., Paiva, M. A. O. S., Silva, J. V. B. D., Guedes, K. P., Gama, T. O., Fernandes, A. T. D. N. S. F., Azevedo, I. G., Morais, P. S. A., Pereira, D. A. G., Pedrosa, R., Lima, J. H. M., & França, E. E. T. (2026). Acute Effect of Inspiratory Muscle Training on Peripheral Tissue Oxygenation Behavior in Individuals With COPD: A Randomized Crossover Study. Physiotherapy Research International. https://pubmed.ncbi.nlm.nih.gov/41738531/