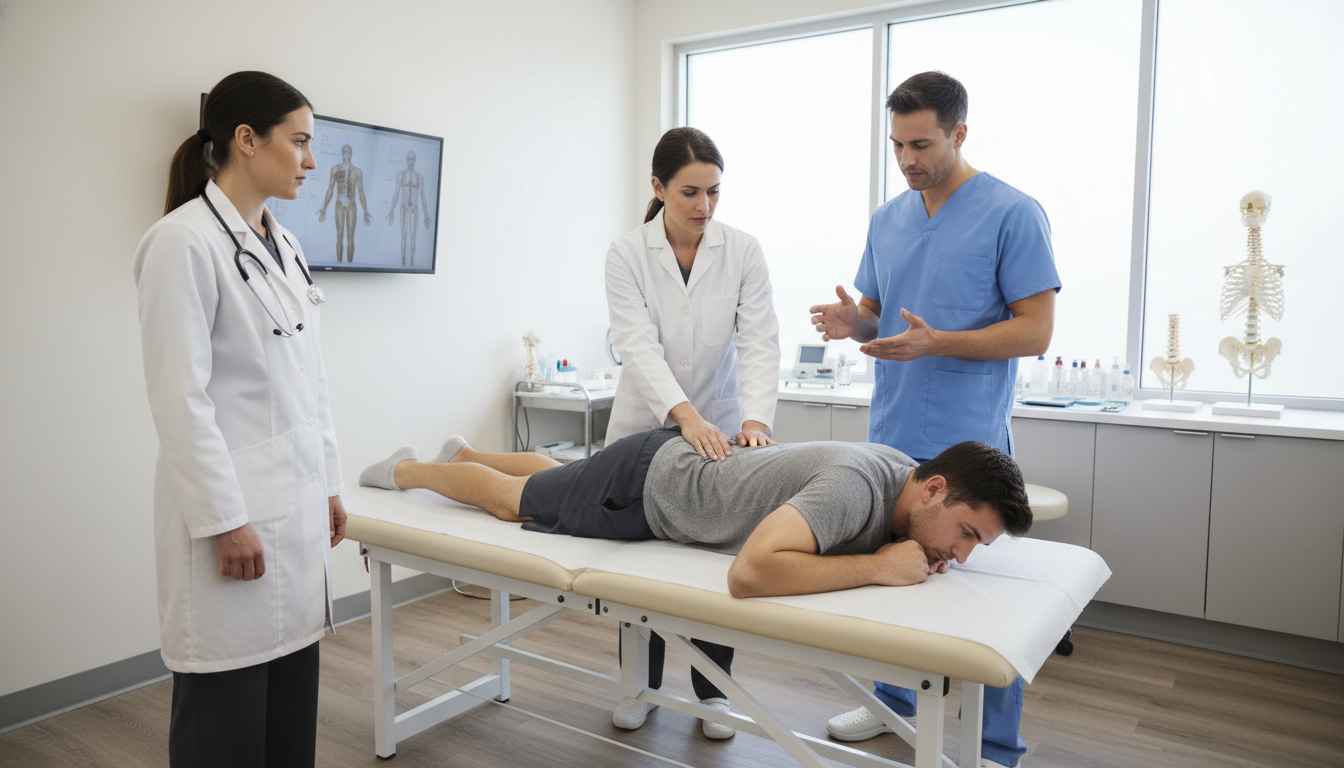
The management of sacroiliac (SI) joint dysfunction has undergone a significant transformation in recent years. Traditionally, SI joint fusion was a major undertaking performed exclusively by orthopedic spine surgeons using invasive approaches. However, the advent of percutaneous posterior-oblique techniques has opened the door for Interventional Pain Management (IPM) physicians to perform these procedures. This shift has sparked a debate regarding “practice creep” and patient safety.
For physiotherapists managing the rehabilitation of these patients, understanding the competency of the operating physician and the specific risks associated with evolving surgical techniques is crucial. A recent prospective multicenter randomized controlled trial (RCT), published in The Spine Journal (2025), addresses these concerns by evaluating the safety profile of IPM physicians trained by spine surgeons.
The Evolution of Sacroiliac Joint Interventions
As technology advances, procedures that once required open surgery are becoming minimally invasive. IPM physicians, who already possess expertise in fluoroscopic-guided injections and ablations, are increasingly adopting percutaneous SI joint fusion. This procedure involves the use of titanium screws combined with synthetic bioactive glass flowable biologics to stabilize the joint.
Despite the potential benefits of increased access to care, spine surgeons have raised valid concerns regarding procedural competency gaps and inconsistent safety oversight in outpatient settings. The core question remains: Can IPM physicians perform these fusions with the same safety profile as traditional surgeons?
Analyzing the Influence of Supervision
The study in question followed 276 adult patients scheduled for SI joint fusion across multiple ambulatory surgery centers between 2020 and 2022. All primary procedures were performed by 47 IPM physicians who had undergone structured training on the percutaneous posterior-oblique technique by a board-certified orthopedic spine surgeon.
The patients were randomized into two distinct groups based on intraoperative supervision:
- Group 1: Supervised directly by a spine surgeon (n=66).
- Group 2: Supervised by a non-spine surgeon, such as a clinical specialist or sales representative (n=210).
The primary outcomes assessed were surgical complications, procedural deviations, and revision rates over a follow-up period of at least 12 months.
outcomes and Clinical Significance
The results provided a stark contrast that highlights the value of mentorship and oversight. In total, the study observed a 3.3% complication rate across the cohort. However, the breakdown reveals the critical nature of supervision:
- Group 1 (Spine Surgeon Supervised): Achieved a 0% rate for complications, deviations, and revisions.
- Group 2 (Non-Spine Surgeon Supervised): Experienced a 4.3% complication rate, a 1.9% deviation rate, and a 2.4% revision rate.
Notably, complications in Group 2 occurred between the second and fifth operative days—a critical window where patients may present to physiotherapy for early mobilization.
Implications for Post-Operative Physiotherapy
For the manual therapist and rehabilitation specialist, these findings are encouraging yet cautionary. The data suggests that IPM physicians can safely perform SI joint fusions when adequately trained and supervised. The structured training by spine surgeons appears to be the key differentiator in outcome success.
When treating a patient post-SI fusion, physiotherapists should be aware of the operative setting and the experience level of the provider. While the overall complication rates are low, the distinction in safety profiles underscores the importance of standardized certification programs. As this minimally invasive technique becomes more prevalent, physiotherapists will play a vital role in monitoring for early post-operative deviations, particularly in the first week of recovery.
References
Chin, K. R., Spayde, E., Costigan, W. M., Raikar, S. V., Navalgund, Y. A., Pannozzo, P., Mukalel, J. J., Siwek, S., Narain, S., Fandos, L., Ky, P., Jackson, S., Yeddu, A., Rock, M., Chang, R., Xia, T., Shahid, A., Kountis, V., Coleman, M. H., … Seale, J. A. (2025). A prospective multicenter randomized controlled trial on safety and procedural competency in SI joint fusion performed by interventional pain physicians trained by a spine surgeon. The Spine Journal. https://pubmed.ncbi.nlm.nih.gov/40383200/