Primary dysmenorrhea is one of the most common gynecological complaints affecting quality of life in women of reproductive age. While traditional management often relies on pharmacological interventions or superficial thermal modalities, emerging evidence suggests a significant role for orthopaedic manual therapy. Specifically, the relationship between the spine, the sacroiliac joint (SIJ), and the Autonomic Nervous System (ANS) offers a compelling avenue for therapeutic intervention. A recent Randomized Controlled Trial (RCT) published in Medicina (2024) provides clinical insight into how SIJ manipulation can influence ANS balance and alleviate menstruation-related symptoms.
The Autonomic Link to Menstrual Pain
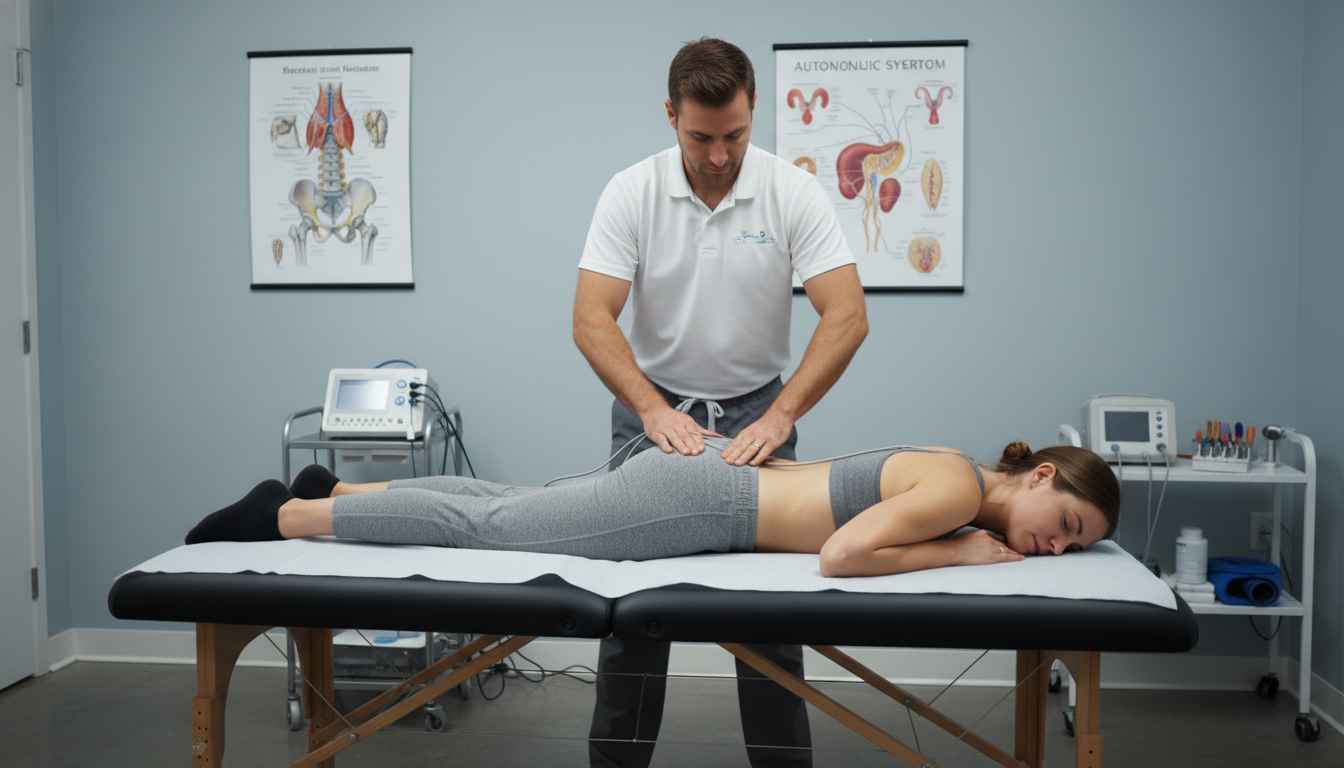
The pathophysiology of primary dysmenorrhea is closely linked to uterine hyperactivity and ischemia, processes regulated by the autonomic nervous system. Dysregulation or imbalance in the ANS can exacerbate pain perception and inflammatory responses. Given the anatomical proximity of the pelvic splanchnic nerves and the sympathetic chain to the lumbosacral region, mechanical dysfunction in the SIJ may contribute to altered somatovisceral reflexes.
Park et al. (2024) investigated this connection by evaluating whether specific manipulation of the SIJ could restore ANS balance—measured via Heart Rate Variability (HRV)—and reduce lower abdominal pain compared to standard conservative care.
Comparing Manual Therapy to Superficial Heat
The study involved 40 participants with primary dysmenorrhea, with 35 completing the final analysis. Participants were randomized into two groups: an experimental group receiving SIJ manipulation (n = 18) and a control group receiving superficial heat therapy (n = 17). Assessments were conducted at baseline and after four weeks of treatment. Crucially, the researchers included an 8-week follow-up to evaluate the sustained effects of the interventions.
Outcome measures included HRV (to assess sympathetic/parasympathetic balance), Visual Analogue Scale (VAS) scores for pain intensity, Pressure Pain Threshold (PPT) of the SIJ, and the Moos Menstrual Distress Questionnaire (MMDQ).
Outcomes: HRV, Pain Thresholds, and Sustained Relief
The results highlighted a distinct physiological advantage for the manipulation group. While both groups experienced a significant reduction in lower abdominal pain (VAS scores), only the group receiving SIJ manipulation demonstrated significant improvements in HRV parameters. This indicates that the manipulation did not merely act as a local analgesic but successfully modulated the autonomic nervous system, shifting the balance towards a more regulated state.
Furthermore, the MMDQ scores, which reflect broader menstrual distress symptoms, showed significantly greater improvement in the manual therapy group compared to the heat therapy group. Perhaps most relevant for clinical practice planning, the reduction in pain and distress was sustained at the 8-week follow-up, suggesting that correcting SIJ dysfunction provides lasting benefits beyond the immediate treatment window.
Implications for Orthopaedic Practice
For physiotherapists, these findings underscore the importance of screening the lumbosacral region in patients presenting with primary dysmenorrhea. While heat therapy remains a valid adjunct for acute symptom management, SIJ manipulation appears to target the underlying autonomic dysregulation. Integrating high-velocity, low-amplitude (HVLA) thrust techniques or specific mobilization of the SIJ into treatment plans offers a potent, non-pharmacological alternative that addresses both the structural and physiological components of menstrual pain.
References
Park, S., Kim, H., Jung, J., & Lee, S. (2024). Effects of Sacroiliac Joint Manipulation on Autonomic Nervous System and Lower Abdominal Pain in Women with Primary Dysmenorrhoea: A Randomized Controlled Trial. Medicina, 60(12), 2110.