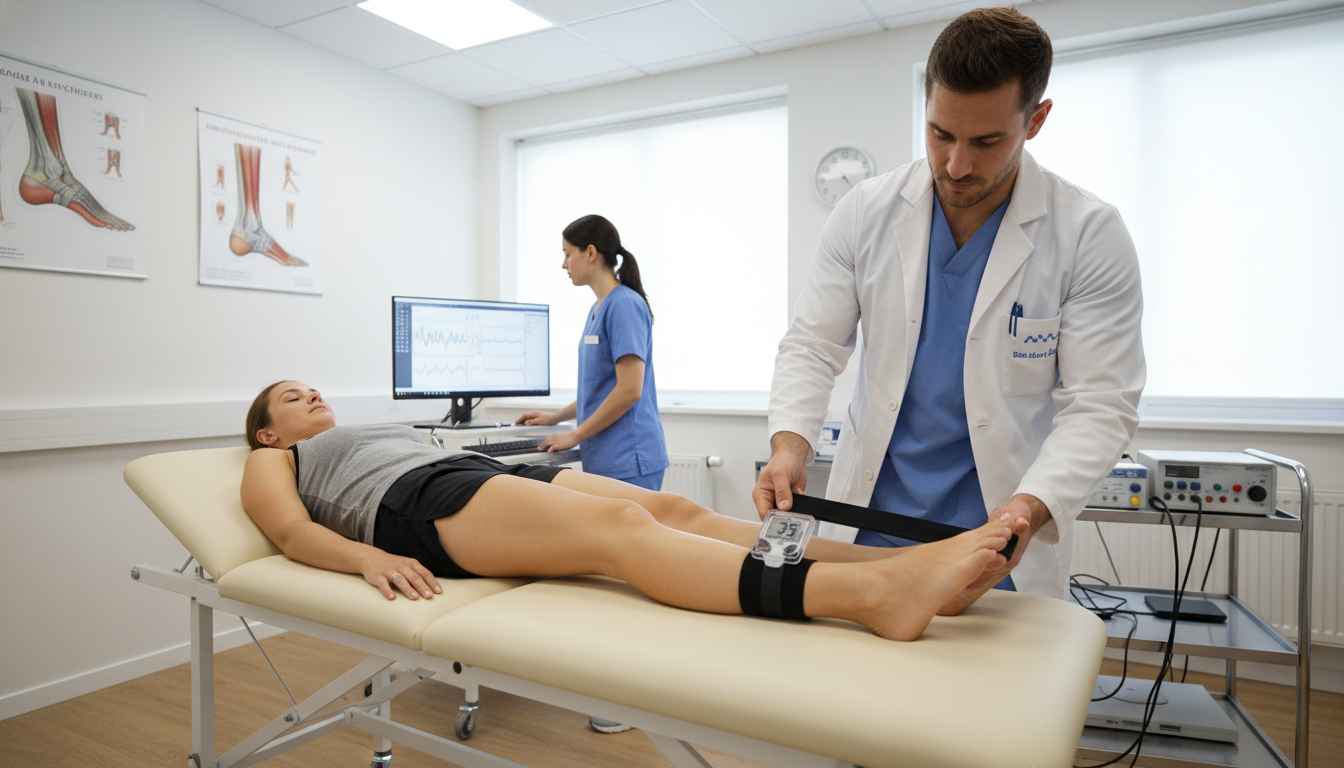
Chronic Ankle Instability (CAI) remains one of the most persistent challenges in sports physiotherapy. Despite rigorous rehabilitation protocols, recurrence rates remain high, often driven by deficits in proprioception, neuromuscular control, and dynamic balance. Recently, tissue flossing—the application of an elastic latex band wrapped tightly around a joint or muscle—has gained popularity as a priming tool to enhance range of motion and functional performance. However, a critical clinical question has remained largely unanswered: does the amount of pressure applied during flossing alter the outcome?
A significant Randomized Controlled Trial (RCT) published in the Journal of Sports Science & Medicine (March 2026) sheds new light on this variable, specifically examining the acute effects of different floss band pressures on multidimensional ankle stability in male patients with CAI.
Investigating Pressure Specificity in Tissue Flossing
The study, led by Chen and colleagues, recruited 42 male participants diagnosed with CAI. To isolate the variable of pressure, participants were randomly assigned to one of three groups: a Medium-Pressure group (MP) receiving 150 mmHg, a High-Pressure group (HP) receiving 200 mmHg, or a Control Group (CG) utilizing a non-compressive bandage. This strict pressure quantification sets this study apart from previous literature that often relied on subjective “perceived tightness” scales.
Researchers evaluated outcomes at baseline and at three post-intervention intervals (5, 25, and 45 minutes). The assessment battery was comprehensive, utilizing the Y-Balance Test (YBT) for dynamic stability, surface electromyography for single-leg landing stability, and specific tests for ankle proprioception and static balance.
Medium vs. High Pressure: Impact on Dynamic Stability
The results provided compelling evidence for the efficacy of tissue flossing, but with a nuanced finding regarding pressure duration. Both the Medium-Pressure (150 mmHg) and High-Pressure (200 mmHg) groups demonstrated statistically significant improvements in YBT composite scores and joint position sense accuracy immediately following the intervention (5 and 25 minutes post-application).
Crucially, electromyographic analysis revealed enhanced lower limb muscle activation during landing tasks in both experimental groups compared to the control. This suggests that the mechanism of flossing extends beyond simple mechanical restrictions or fascial shearing; it appears to induce a neurophysiological response that upregulates muscle recruitment patterns essential for joint protection.
The Clinical “Sweet Spot” for Duration
While both pressures were effective, the Medium-Pressure group (150 mmHg) exhibited a superior duration of effect. Improvements in dynamic stability and neuromuscular metrics in the MP group were sustained up to the 45-minute mark (T3), whereas the benefits in the HP group tended to diminish sooner. The MP group also consistently outperformed the control group across dynamic stability metrics.
For the clinician, these findings suggest that 150 mmHg may represent a therapeutic “sweet spot.” It provides sufficient compression to stimulate mechanoreceptors and induce the reperfusion effects associated with flossing, without the potential diminishing returns or discomfort associated with higher occlusion pressures (200 mmHg).
Clinical Application for Pre-Rehabilitation
Based on this data, physiotherapists should consider implementing floss bands applied at approximately 150 mmHg as a preparatory intervention for CAI patients. The intervention creates a window of enhanced proprioception and neuromuscular control lasting up to 45 minutes. This timeframe is ideal for performing high-level balance training or plyometrics, allowing the patient to train with improved sensorimotor integration.
References
Chen, Y., Zhang, X., Han, B., Mo, T., Gou, Q., Ma, M., Zhang, Q., Guo, C., & Hou, S. (2026). Acute effects of floss band at different pressures on multidimensional ankle stability in patients with chronic ankle instability: A randomized controlled trial. Journal of Sports Science & Medicine. https://pubmed.ncbi.nlm.nih.gov/41710447/