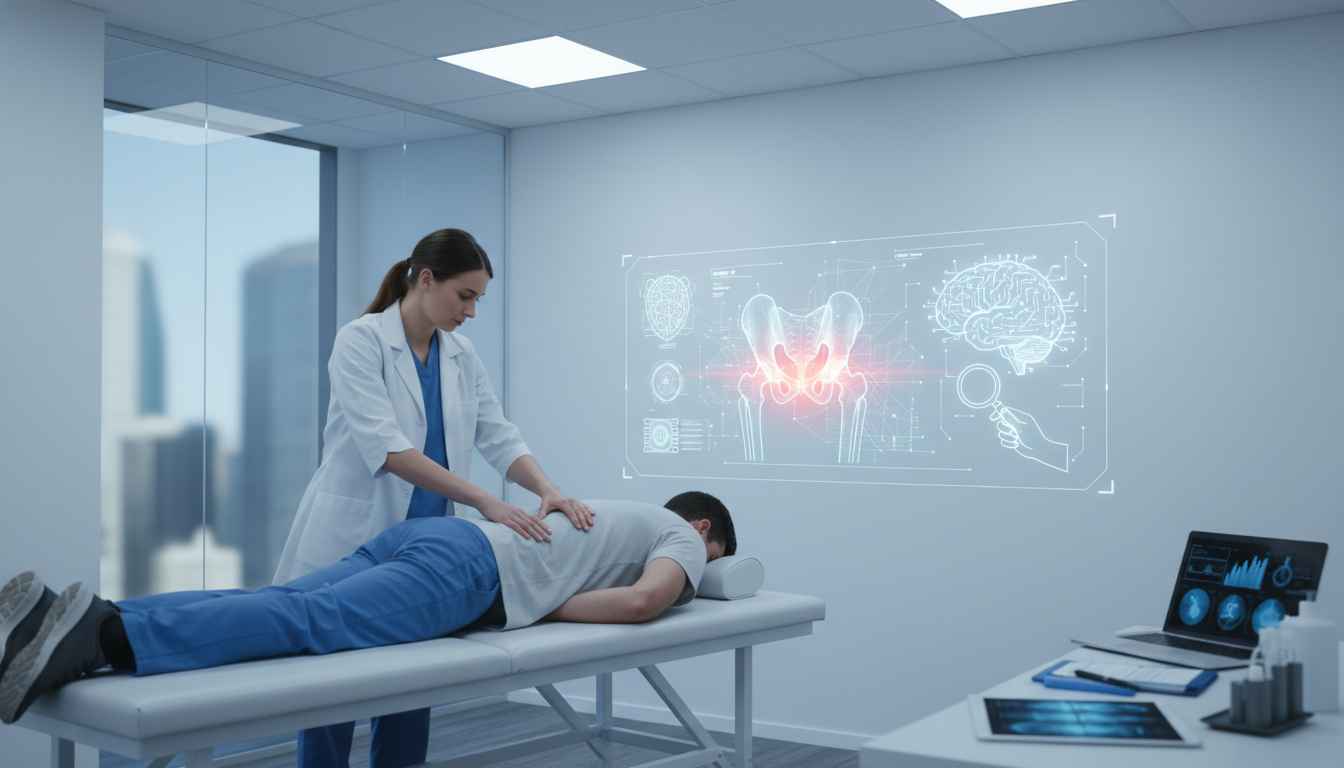
The integration of artificial intelligence (AI) into musculoskeletal diagnostics is rapidly advancing, offering new possibilities for the early detection of complex rheumatological conditions. For physiotherapists, recognizing the signs of axial spondyloarthritis (axSpA) is a critical component of triage and referral. A landmark study published in the Annals of the Rheumatic Diseases in January 2025 has provided robust validation for a deep-learning algorithm designed to detect inflammation in the sacroiliac joints (SIJ) on MRI scans.
The Challenge of Diagnosing Axial Spondyloarthritis
Axial spondyloarthritis, encompassing both radiographic (r-axSpA) and non-radiographic (nr-axSpA) forms, is notoriously difficult to diagnose in its early stages. The current gold standard for identifying active disease involves the detection of bone marrow edema on MRI sequences, specifically utilizing the 2009 Assessment of SpondyloArthritis International Society (ASAS) definition. However, interpretation of these images requires significant expertise and can be subject to inter-reader variability.
To address this, researchers assessed a previously trained deep-learning algorithm against a large external validation set. The study pooled baseline SIJ MRI scans from two prospective randomized controlled trials: RAPID-axSpA and C-OPTIMISE. This created a substantial dataset of 731 patients, comprising a mix of r-axSpA and nr-axSpA presentations.
Methodology: A Robust External Validation
The strength of this study lies in the diversity of its data. The MRI scans were sourced from over 100 clinical sites, utilizing more than 30 different scanners from 5 distinct manufacturers. This heterogeneity is crucial for testing the real-world applicability of AI tools, as image quality and parameters often vary between clinics.
The scans were processed by the deep-learning algorithm, which was blinded to all clinical information. These results were then compared against central evaluations performed by expert human readers (with adjudication in cases of disagreement). The study population was demographically representative of a typical axSpA cohort, with a mean age of 34.2 years and a 69.1% male prevalence.
Performance Metrics: Sensitivity and Specificity
The results offer a promising, albeit nuanced, view of AI capabilities in rheumatology. Upon comparison with human expert consensus, the algorithm demonstrated the following performance metrics:
- Sensitivity: 70% (95% CI 66% to 73%)
- Specificity: 81% (95% CI 78% to 84%)
- Positive Predictive Value (PPV): 84%
- Negative Predictive Value (NPV): 64%
- Absolute Agreement: 74%
The Cohen’s kappa score, a measure of inter-rater reliability, was 0.49. While this represents moderate agreement, it is important to note that human-to-human agreement in SIJ MRI interpretation also varies significantly. The high specificity (81%) and PPV (84%) suggest that when the algorithm flags inflammation, it is highly likely to be present.
Implications for Clinical Practice
For the physiotherapy profession, these findings suggest that AI could soon serve as a powerful triage tool. While the sensitivity of 70% indicates that the algorithm currently misses approximately 30% of positive cases (false negatives), its ability to rule in disease is strong. This technology could assist radiologists in high-volume settings or support clinicians in areas with limited access to specialized rheumatologic imaging expertise.
As these algorithms evolve, they may help reduce the diagnostic delay often experienced by axSpA patients, facilitating earlier referral from physiotherapy clinics to rheumatology for appropriate biologic or medical management.
References
Nicolaes, J., Tselenti, E., Aouad, T., López-Medina, C., Feydy, A., Talbot, H., Hoepken, B., de Peyrecave, N., & Dougados, M. (2025). Performance analysis of a deep-learning algorithm to detect the presence of inflammation in MRI of sacroiliac joints in patients with axial spondyloarthritis. Annals of the Rheumatic Diseases. https://pubmed.ncbi.nlm.nih.gov/39874235/