Acute low back pain remains one of the most common and debilitating conditions encountered in primary care. Traditionally, family physicians have served as the gatekeepers for conservative management, often leading to delayed physical rehabilitation and an over-reliance on pharmacological interventions. However, a progressive shift is occurring in healthcare systems worldwide. A recent pragmatic cluster randomized controlled trial (RCT) conducted in France explored an innovative model of care: empowering physiotherapists to act as first-contact practitioners for patients with acute low back pain.
Shifting the Paradigm: Physiotherapists at the Frontline
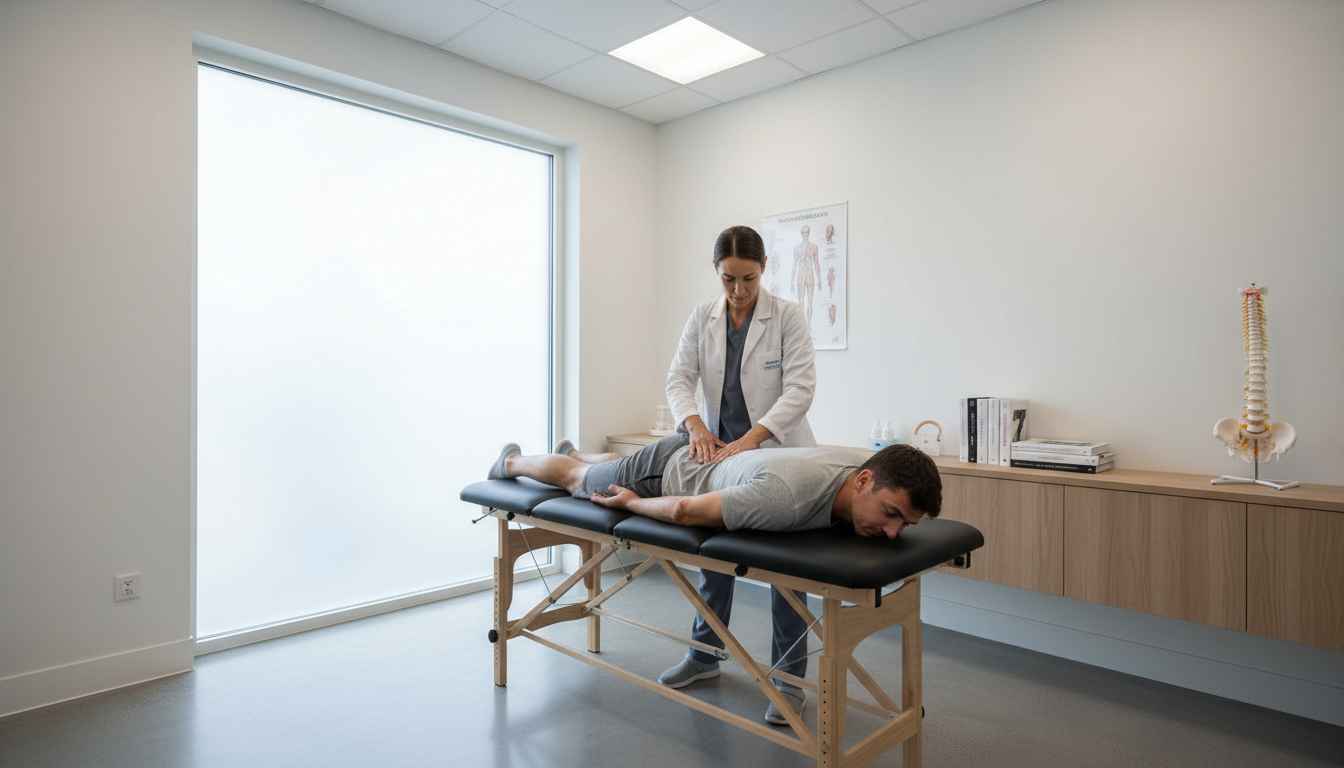
In this newly evaluated advanced practice model, French physiotherapists collaborated closely with family physicians but expanded their traditional scope of practice. Crucially, these first-contact physiotherapists were granted the autonomy to independently assess, diagnose, and manage patients, which included the delegation of medication prescription rights. This multicenter RCT aimed to determine if this first-contact physiotherapy (FCP) model could deliver outcomes comparable to, or better than, usual care provided by a family physician.
Evaluating the Efficacy of the Advanced Practice Model
The study recruited 60 patients, aged 20 to 55, suffering from acute low back pain across six multidisciplinary primary healthcare centers. Participants were randomized to consult either a physiotherapist or a family physician. The primary clinical outcome measured was patient disability at the six-week mark, assessed using the Roland Morris Disability Questionnaire. Secondary outcomes provided a comprehensive view of patient recovery, including pain levels, risk of chronic disability, healthcare resource utilization, wait times, and overall patient satisfaction with the care received. Evaluations were systematically recorded at baseline, six weeks, and twelve weeks.
Clinical Outcomes and Reduced Medication Reliance
The results of the trial are highly encouraging for the advancement of our profession. The adjusted mean difference for disability at six weeks between the two groups was a negligible 0.39 points, which comfortably falls within the established non-inferiority margin based on a 5-point minimal clinically important difference. Furthermore, there were no statistically significant differences regarding disability at three months or pain scores at both the six-week and three-month follow-ups. Notably, the most striking finding was in healthcare resource utilization: physiotherapists prescribed significantly less medication than their physician counterparts (p < 0.001). Patient satisfaction, wait times, and other resource uses remained robust and consistent across both primary care pathways.
Implications for the Future of Orthopaedic Physiotherapy
This landmark RCT is the first of its kind to rigorously evaluate an advanced FCP model that incorporates delegated medical acts, such as prescribing, within a primary care setting. For orthopaedic and manipulative physiotherapists, these findings reinforce our capability to safely and effectively manage acute spinal conditions from day one. By matching the clinical outcomes of family physicians while drastically reducing medication dependence, first-contact physiotherapists can play a pivotal role in curbing the over-medicalization of acute back pain. While larger, appropriately powered studies are required to solidify these conclusions, this research strongly paves the way for a more efficient, conservative-first approach to musculoskeletal primary care triage.
References
Kechichian, A., Desmeules, F., Girard, P., Terrisse, H., Vermorel, C., & Pinsault, N. (2024). Physiotherapists as first-contact practitioners for patients with low back pain in French primary care: a pragmatic cluster randomised controlled trial. BMC Health Services Research.