Understanding Long-Term Outcomes in Stress Urinary Incontinence
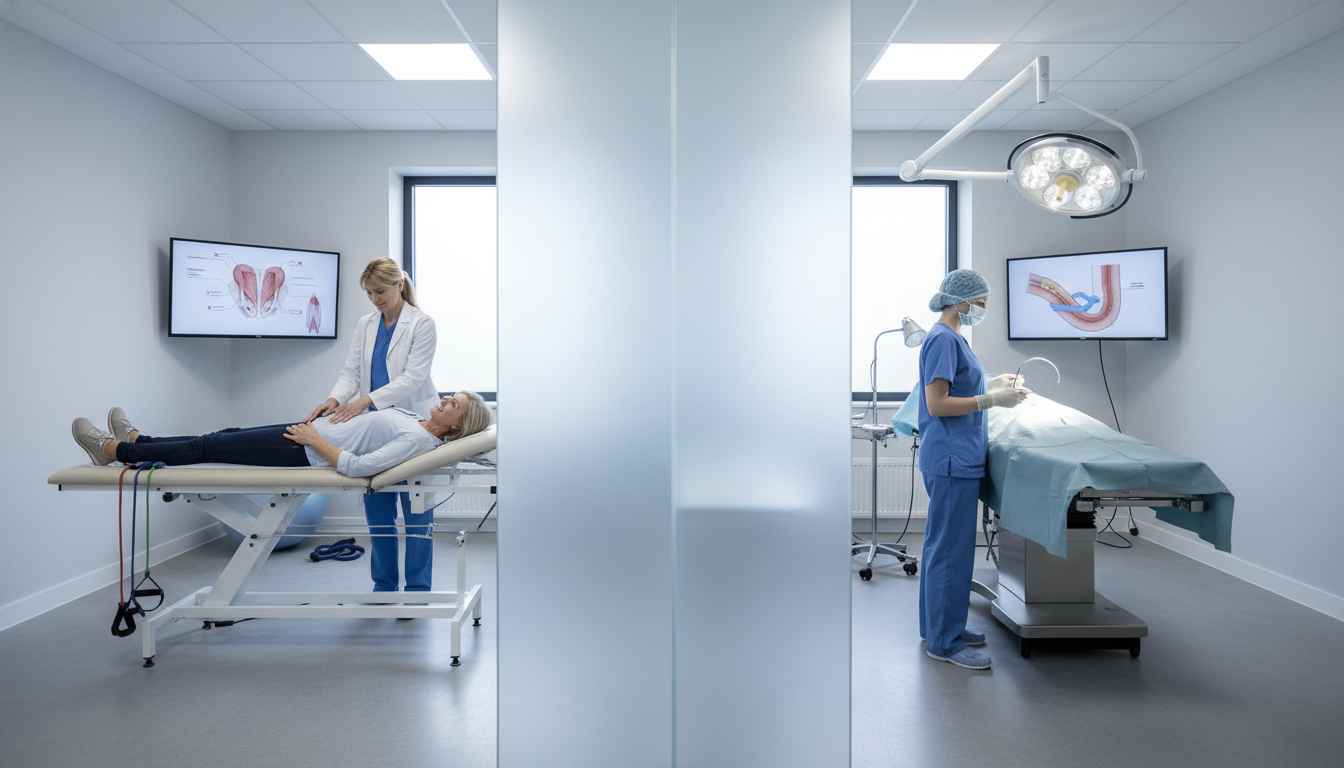
For physiotherapists treating pelvic floor dysfunction, establishing realistic long-term expectations for conservative management is crucial. A recent 12-year follow-up study originating from the PORTRET trial sheds light on the prolonged efficacy of pelvic floor muscle training (PFMT) compared to mid-urethral sling surgery for women with moderate to severe stress urinary incontinence (SUI). By evaluating these long-term outcomes, clinical practitioners can better optimize their treatment plans and guide shared decision-making processes.
High Crossover Rates: From Conservative to Surgical Management
Conducted at the University Medical Centre Utrecht, this observational follow-up aimed to assess subjective improvement over more than a decade. Among the 184 respondents, the most striking finding for rehabilitation professionals was the exceptionally high crossover rate. Approximately 86.9% of the women initially assigned to the physiotherapy group eventually opted for surgical intervention. While intention-to-treat analyses showed no statistically significant differences, post-hoc analyses painted a clearer picture of patient journeys. Women who relied exclusively on physiotherapy reported significantly lower subjective improvement compared to those who underwent surgery initially or following a trial of conservative care. The absolute difference in improvement was staggering, hovering around 50% in favor of surgical intervention.
Re-evaluating the Role of Pelvic Floor Muscle Training
Does this high crossover rate diminish the value of PFMT? Not necessarily. As conservative practitioners, it is vital to contextualize these findings within the clinical pathway of SUI management. Current guidelines continue to advocate for PFMT as a first-line, non-invasive treatment. However, this 12-year follow-up provides essential prognostic data for patient communication. When dealing with moderate to severe cases, patients must be informed that while PFMT is a safe, low-risk starting point, long-term resolution may ultimately require surgical support. Subjective cure rates, decreased perceived severity, and the overall impact of SUI heavily favored the surgical cohorts in this long-term analysis.
Clinical Takeaways for Pelvic Health Physiotherapists
This study reinforces the necessity of timely reassessment and multidisciplinary collaboration. If a patient with moderate to severe SUI does not demonstrate meaningful, sustained improvement with a structured PFMT program, prompt referral for surgical consultation is highly appropriate and evidence-based. Mid-urethral sling surgery, whether performed initially or after a course of physiotherapy, significantly improves subjective outcomes in the long run. By understanding these long-term trajectories, physiotherapists can better guide their patients, managing expectations while fostering an integrated approach to women’s pelvic health.
References
van Oorschot, H. F. C., Tijsseling, D., Labrie, J., & van der Vaart, C. H. (2025). Twelve-Year Follow-Up of a Randomised Controlled Trial Comparing the Effectiveness of Pelvic Floor Muscle Training Versus Mid-Urethral Sling Surgery for Female Moderate to Severe Urinary Incontinence. BJOG : an international journal of obstetrics and gynaecology. https://pubmed.ncbi.nlm.nih.gov/39931871/